
Q&A with Salimah Walani: leveraging newborn screening to improve access to clubfoot treatment
We sat down with Salimah Walani, Global Policy and Advocacy Advisor at MiracleFeet, to discuss leveraging newborn screening and birth defects surveillance systems to improve access to clubfoot treatment drawing from MiracleFeet’s partner program in the Philippines as an example. Here’s what she had to say.
Q: Salimah, set the stage for us. What do the terms newborn screening and birth defects surveillance mean and how are they linked to improving early detection, referral, and access to treatment for babies born with clubfoot?
A: Newborn screening (NBS) is a general term that refers to the process of conducting screening tests (e.g., biochemical blood test, hearing test) within the first couple of days of a child’s life to identify certain health conditions that can benefit from prompt treatment. Bloodspot or biochemical screening is a type of newborn test that involves collecting a few drops of blood from a baby’s heel, which is then tested in a lab for genomic conditions for genetic, metabolic, endocrinologic, hormonal, and blood disorders. Although NBS programs are widespread in high-income countries where nearly every baby’s blood is tested for several conditions, the implementation of NBS in low- and middle-income countries (LMICs) is highly variable and not well-established.
Birth defects surveillance (BDS) is a type of public health surveillance which involves ongoing collection and analysis of data related to birth defects prevalence. BDS systems may be hospital- or population-based and provide useful information for policy making, resource prioritization, and program implementation. Ideally, a BDS system, even if small, should be linked to care programs through well-developed referral pathways, allowing babies with congenital anomalies to receive healthcare services in a timely and reliable manner.
However, the reality is that birth defects surveillance programs are rare in LMICs and where they are present, they are limited because, they: a) mainly cover births in select urban hospitals, b) include only a few structural birth defects, and c) lack established referral and follow-up pathways.
Q: To help understand this within a specific context, can you describe the recent developments in the Philippines, a country that is launching a nation-wide strategy to improve access to treatment of select congenital anomalies, including clubfoot?
A: The Philippines is a lower-middle income country with a population of about 117 million. In 2004, Philippines passed the Republic Act 9288 (an act promulgating a comprehensive policy and a national system for ensuring newborn screening) to provide governance and framework for implementation of a nation-wide newborn screening (bloodspot testing) program. As of 2023, the Philippines’ NBS (bloodspot) program covers more than 7,000 hospitals and birthing centers, screening almost 95% of all births in the country for 29 conditions. In July 2023, the Philippines Department of Health approved the expansion of the country’s NBS to initiate a population and facility based BDS project. Dr. Carmencita Padilla, a well-known scientist and global leader in NBS and birth defects, is leading this effort.
The program has four phases. The first phase focuses on visible and structural birth defects. The four conditions included are: neural tube defects, orofacial clefts, abdominal wall defects and clubfoot.
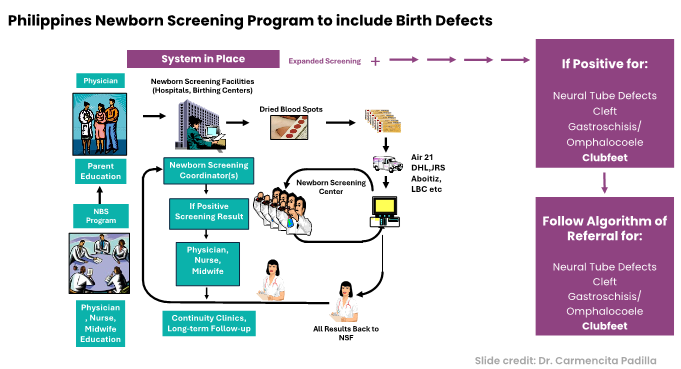
A steering committee and a coordinator have been appointed to create a data collection system/registry and an algorithm for reporting, referring, and treating babies identified with these four conditions. The newly established systems will be pilot tested in the National Capital Region (NCR) before they are implemented nationwide over the next few years.
MiracleFeet and our partner, Philippine NGO Council on Population, Health, and Welfare, Inc. (PNGOC), are providing technical and administrative support to the clubfoot component of the BDS to facilitate the data-collection process and development of referral to care pathways leading to enrollment in clubfoot treatment.
Q: What can we learn from the Philippines experience?

A: MiracleFeet’s mission is to increase access to evidence-based treatment for children born with clubfoot in LMICs through partnerships with local healthcare providers. One of the main barriers to care in LMICs is the lack of a system to identify and refer newborns with clubfoot to a treatment clinic. The newborn period (first 28 days of life) provides an opportunity for early detection of clubfoot and increasing treatment adherence and success rates. Although very few LMICs have well-established NBS or BDS programs, whenever possible, we must look for and actively integrate with these systems in our program countries, facilitating early detection processes and establishment of referral to care pathways. Additionally, whenever possible, we should place the clubfoot care agenda in the maternal and newborn health (MNH) systems at national and global levels. Recognizing the importance of the newborn period in improving child survival and well-being, many countries and global organizations have invested significant resources in designing healthcare systems to improve the health outcomes of moms and babies.







